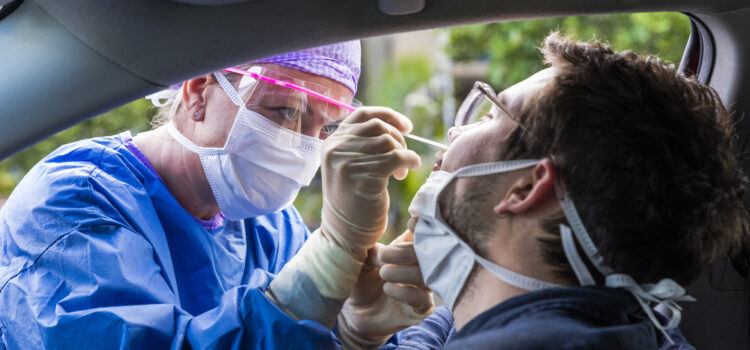
The California Department of Public Health released updated testing guidance Tuesday that focuses on testing hospitalized individuals with signs or symptoms of COVID-19 and people being tested as part of the investigation and management of outbreaks, including contact tracing.
The testing guidance also prioritizes individuals who have COVID-19 symptoms and individuals without symptoms who fall into high-risk categories, including people who live and work in nursing homes, homeless shelters and prisons, healthcare workers, and patients in hospitals.
“Testing is a critical tool that helps us diagnose and treat those who become infected by COVID-19,” said California Health and Human Services Secretary Dr. Mark Ghaly. “Testing also helps us understand how COVID-19 moves through our communities so we can identify areas where transmission is occurring.”
The new testing guidance breaks down testing priories into four tiers. As mentioned above, the tier one priority will be for hospitalized individuals with COVID-19 symptoms.
Tier two priority will be for all other individuals with COVID-19 symptoms, and individuals who are asymptomatic, who fall into one of many categories, including individuals who live in higher risk congregate care facilities; work in the health care sector; work in a congregate care facility; and provide care to an elderly person or a person with a disability in the home.
Tier three priority is for individuals who work in retails or manufacturing sectors; in food services sector; in agricultural or food manufacturing sector; and in the education sector.
Tier Four would be implemented when the state’s testing turnaround time, as monitored by CDPH, is less than 48 hours.
The new guidance ensures Californians who most need tests get them even if there are limited supplies, according to a news release.
Ghaly said at a press conference Tuesday that California’s testing capacity has increased exponentially in recent months.
In the last month in Kern County alone from mid-June to mid-July, there have been more than 47,000 tests conducted, which is far more than the nearly 30,000 tests conducted between mid-May to mid-June.
However, many challenges arise with an increase in testing.
“At the same time, new national supply chain challenges and large volumes of specimens sent to commercial laboratories have resulted in growing delays in processing times,” said Ghaly. “Consequently, it is critical we continue to be deliberate and creative about testing. We must do this so that testing is readily available and affordable to those who need it, especially those communities experiencing the worst impacts of COVID-19 and those who are at the highest risk.”
California’s Testing Task Force, which was launched in April, has created testing locations where there were none, expanded laboratory capability and helped build a testing supply pipeline, scaling up from just 2,000 tests per day to more than 100,000 tests per day throughout California, according to a news release.
The new leaders of the task force will recommend testing priorities, continue to create equitable access to testing and support for state-operated community testing sites, and review options to lower overall testing costs.
To help ensure that testing is available to all Californians, the state is working with health insurers to provide reimbursement for testing and with private providers to create additional in-office testing capacity, according to a news release.
With more providers performing tests in the office rather than referring patients to labs or testing sites, the state would have more resources to focus on under-served and high-risk populations. The state is preparing to file emergency regulations that will classify COVID-19 testing as medically necessary urgent care for essential health workers and people with symptoms of or possible exposure to COVID-19.
Ghaly said, “Testing is a responsibility of our entire healthcare delivery system. Clinics, doctors, and other care sites should provide convenient testing to their patients who need a test.”
For more information on the new guidance, head to CDPH.ca.gov and for more information on testing sites in Kern County, head to kerncounty.com.